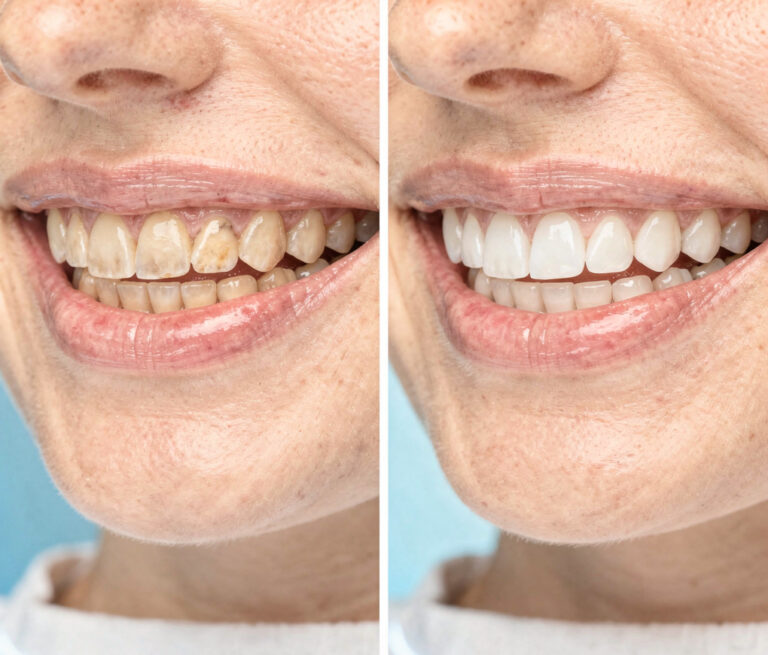
Introduction: Why Maintenance Determines Your Investment
Porcelain veneers are restorations that last decades, but longevity is not automatic. Clinical studies demonstrate that 95% of veneers maintain full functionality after 10 years, but this statistic is not universal—it depends entirely on how you care for your restorations.
What most patients don’t understand is that daily maintenance can extend your veneer lifespan from 12 years to 20+ years, or shorten it dramatically if you adopt destructive habits.
This guide breaks down every technical aspect of veneer care, backed by current dental research, so you can make informed decisions that protect your investment.
Part 1: The Science Behind Maintenance
Why Veneers Require Specific Care
Veneers are multi-layered structures composed of:
- Glass-ceramic core (primary material: feldspathic porcelain or lithium disilicate)
- Resin bonding layer (adhesive that holds the veneer to the natural tooth)
- Natural tooth underneath (your original bone structure)
Unlike natural enamel, which has self-healing properties and can remineralize, veneers are inert restorations. Once fractured or debonded, they cannot self-repair—they must be replaced.
Additionally, the critical weak point is the margin (the edge where the veneer meets the gum and natural tooth). This interface is vulnerable to:
- Bacterial plaque accumulation (which weakens the adhesive bond)
- Saliva infiltration (which gradually degrades the cement)
- Acid exposure (from food, beverages, and gastric acids)
- Excessive bite forces (which create stress at the margins)
Part 2: Professional Brushing Technique
The Right Toothbrush: Type and Characteristics
Soft-Bristled Toothbrush:
Your dentist probably recommended “soft” or “extra soft” brushes. This is not a casual suggestion—it’s a technical requirement.
- Why: Hard-bristled brushes create microabrasions (microscopic scratches) on the porcelain surface. After 6-12 months of hard-brush use, the surface loses its natural shine and reflects less light, appearing opaque or aged.
- Replacement: Change your toothbrush every 3 months or when bristles begin to fray. Worn bristles become abrasive, even if they started “soft.”
Electric vs. Manual Toothbrush:
Clinical studies show that electric toothbrushes produce less microabrasion than manual brushes because:
- They provide consistent motion without pressure variation
- Many have pressure sensors that alert if you’re pressing too hard
- The vibration speed is predictable and controlled
Recommendation: If you brush with heavy pressure, an electric toothbrush with pressure detection (like Philips Sonicare or Oral-B Pro) better protects your veneers.
Correct Brushing Technique
Circular vs. “Sawing” Motion:
Many people brush horizontally (back and forth), which applies lateral pressure that damages both gum tissue and veneer margins.
Correct technique:
- Angle the brush at 45 degrees to the gum line
- Use gentle circular motions starting from the gum toward the tooth (not horizontal)
- Minimal pressure: Your hand should rest lightly—if you feel pressure, you’re pressing too hard
- Duration: Minimum 2 minutes per session (divided: 30 seconds per quadrant)
- Focus on margins: Pay special attention to the line where the veneer meets the gum—plaque accumulates most here
Why pressure matters:
- Excessive pressure = microlesions in the gum = gum recession
- Gum recession = veneer margin exposure = weakened bond = debonding risk
Brushing Frequency
Brush twice daily—morning and night.
Why not three times?
While brushing after meals is common practice, doing so shortly after consuming acidic foods (citrus, wine, soft drinks) temporarily softens enamel, making it more vulnerable to friction damage.
Optimal protocol:
- Morning: Brush immediately after waking (2 minutes)
- After food/beverages: Rinse with water (don’t brush, especially if it was acidic)
- Night: Wait 30 minutes after dinner, then brush thoroughly (2 minutes)
- Additional benefit: Nighttime rinsing is critical because during sleep there’s less saliva production, which is your natural defense against bacteria
Part 3: Toothpaste Selection and Use
What Characteristics Your Toothpaste Should Have
Non-Abrasive (Critical):
Toothpaste abrasiveness is measured on a scale called RDA (Relative Dentin Abrasivity). For veneers:
- Ideal: RDA < 70
- Acceptable: RDA 70-100
- AVOID: RDA > 100
High-RDA pastes include:
- Whitening/bleaching toothpastes
- Charcoal-activated pastes
- Pastes with polishing powders
- “Natural” pastes with salt or baking soda
These products erode the outer shine layer of veneers, leaving them opaque in 6-12 months.
Fluoride-Containing (Essential):
Fluoride strengthens the enamel underlying your natural tooth under the veneer. Even though the veneer protects most of the surface, the margin exposes natural enamel vulnerable to decay.
- Recommended concentration: 1,000-1,500 ppm fluoride
- Check label: Verify the paste says “fluoride”
Without Natural Oils (Important for bonding):
Some “natural” dental products contain coconut oil, tea tree oil, or other oils. These can:
- Penetrate the adhesive interface (veneer margin)
- Gradually degrade the resin cement
- Create space for bacterial infiltration
Recommended formula:
Look for pastes labeled “non-abrasive fluoride toothpaste for veneers” or ask your dentist for a specific recommendation. Some examples:
- Sensodyne Pronamel (RDA ~60)
- Colgate Sensitive Pro-Relief (RDA ~70)
- Professional veneer-specific formulas
Quantity and Frequency of Application
A pea-sized amount is sufficient. More paste doesn’t clean better; it only increases unnecessary fluoride exposure.
Part 4: Advanced Flossing Technique
Why Flossing Is Critical to Longevity
Thirty percent of your tooth surface (interproximal spaces and gum line) is unreachable by a toothbrush. This area accumulates the densest plaque, leading to:
- Gum inflammation: Red, swollen gum that bleeds during flossing
- Gum recession: Gum line retreats, exposing the veneer margin
- Bond weakening: When the margin becomes exposed, saliva and bacteria infiltrate the adhesive interface
- Underlying decay: Develops beneath the veneer, compromising tooth structure
Studies show that daily flossing maintains 95% of gum health compared to only 40% without regular flossing.
Correct Flossing Technique
Common error: “Snapping” the floss
Many people place floss between teeth and snap it upward briskly. This can:
- Damage the gum (causing small wounds)
- Dislodge the veneer margin if incorrect pressure is applied
- Accelerate gum recession
Correct technique:
- Use 45 cm (18 inches) of floss—wrap most around your middle fingers, leaving ~2.5 cm of taut floss between your fingers
- Guide gently: Introduce floss between two teeth with a gentle sawing motion (not brute force)
- C-shape: Once between the teeth, gently wrap the floss around one tooth in a “C” shape
- Vertical motion: Slide the floss from top to bottom (not side-to-side). This motion is gentle on the gum and effective at removing plaque
- Reach below the gum line: Move the floss slightly below the gum line (1-2 mm), where the densest bacterial plaque accumulates. This is the critical point.
- Repeat for each space: Each interproximal space requires its own downward cleaning motion
- Never “cut” through the veneer margin: If you feel resistance, don’t force. Back off and retry at a slightly different angle.
Duration: 2-3 minutes total (after nighttime brushing)
Alternatives to Traditional Floss
If traditional floss is uncomfortable or risky with your veneers:
Interdental Brushes:
Available in various sizes, these small brushes fit between teeth. Advantages:
- Less pressure on veneer margins
- Easier to control
- Equal or superior cleaning compared to floss
Water Flossers:
Use water pressure to remove plaque. Recent studies show efficacy comparable to or superior to traditional floss. Additional advantages:
- Don’t damage the gum when used correctly
- Easier for patients with limited manual dexterity
- Ideal if you have bruxism (gums tend to be inflamed)
Dental Picks:
Small rubber or plastic tools that gently scrape between teeth. Less effective than floss or interdental brushes, but better than nothing.
Gum Bleeding: When It’s Normal
If your gums bleed during flossing:
- First 1-2 weeks: Mild bleeding is normal (means your gum was inflamed; regular flossing normalizes inflammation)
- After 2 weeks: Bleeding should decrease. If it continues, consult your dentist.
- Never stop flossing due to bleeding: Stopping worsens inflammation. Continue gentle flossing—bleeding will cease in 7-10 days.
Warning signs:
- Persistent bleeding after 3 weeks
- Severe swelling, bright red, or pus
- Extreme pain or sensitivity
These symptoms may indicate periodontal disease requiring immediate professional intervention.
Part 5: Foods, Beverages, and Habits That Deteriorate Veneers
Hard Foods: Fracture Risk
Foods to avoid or consume with caution:
- Ice: Microfractures begin when ice freezes and expands in microscopic porcelain deficiencies. After 5-10 years of ice-chewing, many veneers develop visible cracks. [Avoid completely]
- Hard candy (lollipops, hard candies): Applies concentrated forces at specific points. [Avoid]
- Unpopped popcorn kernels: Create exceptional impact forces. [Avoid]
- Chicken bones, ribs, olive pits: [Avoid biting directly; remove with back molars]
- Raw apples, carrots: Safe to eat, but cut into small pieces and chew with back molars, never with front teeth where veneers are
- Hard bread, baguettes: Crunchy bread can apply lateral pressure to veneers; cut or chew gently
Staining Beverages: Porosity Science
Although porcelain is non-porous compared to composite bonding, the veneer margins (where it touches natural enamel) CAN stain.
Problematic beverages and why:
- Coffee, black tea: Contain tannins that stain exposed enamel at margins. Visible effect after 3-6 months of daily consumption without preventive measures.
- Red wine: Anthocyanin pigments penetrate deeply into the marginal interface. One glass weekly = visible discoloration in 1 year.
- Cola drinks, dark beverages: Acid + pigment = double damage. Acid weakens the adhesive bond while pigments stain.
- Cranberry, pomegranate, red fruit juices: Highly concentrated natural pigments.
- Curry, tomato sauces: Spice pigments can stain with cumulative effect over years.
Mitigation strategy:
- Use a straw: For dark beverages, drink through a straw to avoid contact with front teeth
- Drink water afterward: Water dilutes and rinses pigments
- Don’t brush immediately: Wait 30 minutes (especially with acidic beverages)
- Professional cleaning: Every 6-12 months, request professional cleaning that can gently polish margins without damaging veneers
Dietary Acids: The Invisible Risk
Much less obvious than hard foods, but equally destructive:
Acid sources:
- Vinegars: Balsamic, white wine, apple cider
- Citrus: Lemon, lime, orange (especially in water or beverages)
- Dried fruits: Raisins, dried cranberries, dried apricots
- Sports drinks: High citric acid content
- Acid reflux: Untreated GERD—gastric acid at night deteriorates adhesives and margins
How acid damages veneers:
- Demineralizes underlying enamel
- Weakens resin adhesive components
- Expands the marginal interface, allowing bacterial infiltration
- Over 10+ years, can drastically compromise longevity
Protection protocol:
- Rinse with water after consuming acidic foods
- Wait 30-60 minutes before brushing (your enamel is temporarily soft after acid exposure)
- If you have GERD, speak with your physician about treatment options
Part 6: Destructive Habits and Bruxism
The Impact of Bruxism on Longevity
This is the most important factor affecting your veneer lifespan.
Clinical data:
A study of 323 veneers published in a dental research journal found:
- Patients WITHOUT bruxism: Fracture/debonding rate = 4%
- Patients WITH bruxism, no night guard: Fracture/debonding rate = 30-35%
- Patients WITH bruxism AND night guard: Fracture/debonding rate = 12-15%
What this means in real longevity:
- No bruxism = 12-18 years average
- Bruxism without guard = 5-7 years average
- Bruxism + night guard = 15-20 years average
Do you have bruxism?
Warning signs:
- Your partner mentions you grind your teeth at night
- You wake with jaw pain
- Your natural teeth show wear facets (flat, rounded edges)
- You have visible fracture lines in your teeth
- Frequent morning migraines
- Visible wear on older dental work
If you have bruxism: A night guard is NON-NEGOTIABLE
A hard acrylic night guard ($200-400) is a tiny investment compared to replacing veneers ($900-2,500 x multiple teeth = $5,000-15,000+).
Other Destructive Habits
Nail-biting (Onychophagia):
- Creates leverage forces that gradually debond veneers
- Introduces oral bacteria into the adhesive interface
- Causes microfractures at veneer corners
- If you have this habit, use a physical barrier: cotton gloves at night, or bitter-tasting nail polish that discourages biting
Opening bottles or packages with teeth:
- Obvious risk but surprisingly common
- Creates lateral forces veneers aren’t designed for
- Causes acute fracture in ~5% of cases
Biting pens, pencils:
- Similar risk to above
- Repeated microabrasions weaken veneer integrity
“Playing” habits:
- Constantly running your tongue over margins
- Attempting to “wiggle” veneers with your tongue
- Pressing veneers with your fingers
Part 7: Warning Signs and When to Consult Your Dentist
Symptoms Requiring Immediate Professional Attention
Color change or staining:
- Brown or gray discoloration around margins = bacterial infiltration or adhesive leakage
- Black spot = possible underlying decay
Action: Consult within 1-2 weeks. Left untreated, decay can compromise tooth structure.
Increased sensitivity:
- Cold or temperature sensitivity you didn’t have before
- Indicates the margin is compromised, exposing dentin
Action: Consult within 1 week. If detected early, this can be sealed easily.
Change in fit or adjustment:
- Veneer feels loose or mobile
- Visible movement of veneer under digital pressure
- “Clicking” sound when chewing
Action: Consult immediately (within 3-5 days). A debonded veneer risks acute dental infection.
Gum changes:
- Gum recession (gum line drops, exposing more root)
- Persistent swelling, bleeding that doesn’t cease after 3 weeks of daily flossing
- Abscess (swelling with pus)
Action: Consult within 1-2 weeks. Recession affects marginal veneer longevity.
Visible fracture or chip:
- Small crack at corner or edge
- Chip of porcelain visible
Action: Consult within 1 week. Small fractures can be repaired easily; ignoring allows them to expand.
Changes in bite or occlusion:
- Your bite feels different, or you touch on one side first
- Clicking or popping in jaw joint (TMJ)
Action: Consult within 1-2 weeks. This could indicate a veneer has loosened.
Symptoms That Can Wait Until Your Routine Appointment
- Small opaque area or loss of shine
- Minor color discoloration that’s not progressing
- Cosmetic concerns without physical symptoms
Part 8: Professional Cleaning and Maintenance Scheduling
Recommended Professional Cleaning Frequency
Average patients with good oral hygiene: Every 6 months
Reason: Oral bacteria create tartar (calculus) that hardens below the gum line. This accumulation weakens adhesion and causes gum inflammation.
Patients with periodontal disease, implants, or bruxism: Every 3-4 months
Patients with EXCELLENT oral hygiene and no risk factors: Every 9-12 months (though 6 months is still optimal)
What to Expect at Professional Cleaning
Ultrasonic scalers: Your hygienist will use an ultrasonic scaler to remove tartar. These are safe for veneers when used correctly.
Polishing: A non-abrasive polishing agent specified for veneers will be applied. Professional dentists do NOT use standard abrasive polishing powders.
Visual examination: Your dentist will visually examine veneer margins on each tooth, looking for early signs of weakening or infiltration.
Radiographs (every 1-2 years): Periapical bite-wing radiographs can detect underlying decay before it’s visible.
Oral hygiene instruction: If needed, you’ll be taught improved flossing or brushing technique.
Part 9: Special Care After Dental Procedures
After Professional Cleaning
- Avoid hard or sticky foods for 24 hours: Your saliva is slightly compromised after cleaning
- Follow your normal care routine: You don’t need to wait; brush and floss normally after 4-6 hours
After Veneer Repair
If your dentist repaired a damaged veneer with composite filling:
- Avoid hard foods for 48 hours: Freshly applied composite needs time to fully cure
- Return to standard protocols: After 48 hours, resume your normal routine
After Veneer Replacement
If they replaced a veneer completely:
- The new veneer is fully cured the same day: Modern resin adhesives polymerize immediately under UV light
- Wait 1 hour before eating: To allow the adhesive to fully harden
- Temporary sensitivity is normal: May last 3-14 days
Part 10: Real Longevity Data: Evidence-Based Clinical Information
Survival Rates by Porcelain Type
Feldspathic Porcelain (most common, most affordable):
- 94.4% survives 5 years
- 93.5% survives 10 years
- 85.7% survives 15 years
- 82.9% survives 20 years
Lithium Disilicate Porcelain (eMax) (more durable):
- 98% survives 5 years
- 95% survives 10 years
- 91% survives 15 years
- 87% survives 20 years
Minimal-Prep Veneers:
- 100% survives 9 years (in newer studies)
Factors That Improve Longevity
| Factor | Longevity Impact |
|---|---|
| Bruxism controlled (with guard) | +5-7 years |
| Excellent oral hygiene (daily floss + 2x brushing) | +3-5 years |
| Absence of destructive habits | +3-4 years |
| Professional cleanings every 6 months | +2-3 years |
| eMax material vs feldspathic | +3-5 years |
| Avoid dark beverages/acids | +1-2 years |
| Primarily soft/normal diet | +2-3 years |
Factors That Shorten Longevity
| Factor | Longevity Impact |
|---|---|
| Bruxism without guard | -5-8 years |
| Poor oral hygiene | -4-6 years |
| Destructive habits (nail-biting, ice-chewing) | -3-5 years |
| Irregular cleanings (1-2x yearly) | -2-3 years |
| High-acid/dark beverage diet | -2-4 years |
| Smoking | -1-2 years |
| Untreated periodontal disease | -5-10 years |
Part 11: Complete Maintenance Regimen (Executive Summary)
Daily Routine (5 minutes)
Morning:
- Brush 2 minutes with soft-bristled brush, non-abrasive paste
- Rinse with water for 10 seconds
- Rinse with alcohol-free mouthwash (30 seconds)
Night (after dinner + wait 30 min):
- Brush 2 minutes with gentle circular technique
- Floss or use interdental brushes for 2-3 minutes
- Rinse with alcohol-free mouthwash
Weekly Routine (0 additional minutes, awareness only)
- Visual inspection of veneers in natural light
- Look for color changes, cracks, or different-appearing margins
- If you have bruxism, confirm you wore your night guard 5-7 nights
Monthly Routine (1-2 minutes)
- If you have bruxism, inspect your night guard for cracks
- Check your habits: Have you been chewing ice, biting nails, or opening bottles with teeth?
- Evaluate beverage intake—have you increased coffee or wine consumption?
Annual Routine (1 appointment)
- Professional cleaning every 6 months (ideally)
- Complete dental exam of your veneers
- Radiographs to detect underlying decay
- Hygiene instruction if necessary
Conclusion: Your Veneers Can Last 20+ Years
The evidence is clear: Veneers are a long-term investment that survives decades with proper care.
The difference between a patient whose veneers last 7 years and another whose last 20+ years isn’t the material or dentist (though both matter). It’s the daily commitment to oral hygiene, avoidance of destructive habits, and regular professional maintenance.
Invest 5 minutes daily now to protect a thousands-of-dollars investment. Your future smile will thank you.
References and Cited Studies
Alghazzawi, T. F. (2024). Clinical Survival Rate and Laboratory Failure of Dental Veneers. Journal of Dental Research, systematic review of survival rates.
Whitsdental (2025). Research on porcelain microabrasion with hard-bristled brushes.
Clinical comparison: efficacy of electric vs manual toothbrushes in patients with aesthetic restorations.
RDA scale for toothpaste abrasivity in restorations.
Protocols for optimal toothpaste quantity.
Studies on efficacy of daily flossing in gum maintenance (95% vs 40%).
Efficacy of water flossers compared to traditional floss.
Granell-Ruíz, M., et al. (2013). Influence of bruxism on survival of porcelain laminate veneers. Journal of Dental Research, 323 veneers studied over 3-11 years.
Alghazzawi, T. F. (2024). Long-term survival rates of feldspathic porcelain.
Studies on longevity of lithium disilicate porcelain (eMax).